Key takeaways
In the U.S., 28.7% of older adults fall each year, leading to 3 million emergency room visits and a 30% increase in death rates from falls over the past decade.
Fall prevention strategies for seniors include technology, education, physical therapy, and safety devices, with medication review being a common tactic to mitigate fall risk.
Common reasons seniors fall include diminished eyesight and hearing, loss of balance and flexibility, weakened muscle and bone strength, and medication side effects.
A fall risk assessment for seniors involves questions and physical tasks to determine the likelihood of falling, with the CDC recommending an annual assessment for those aged 65 and older.
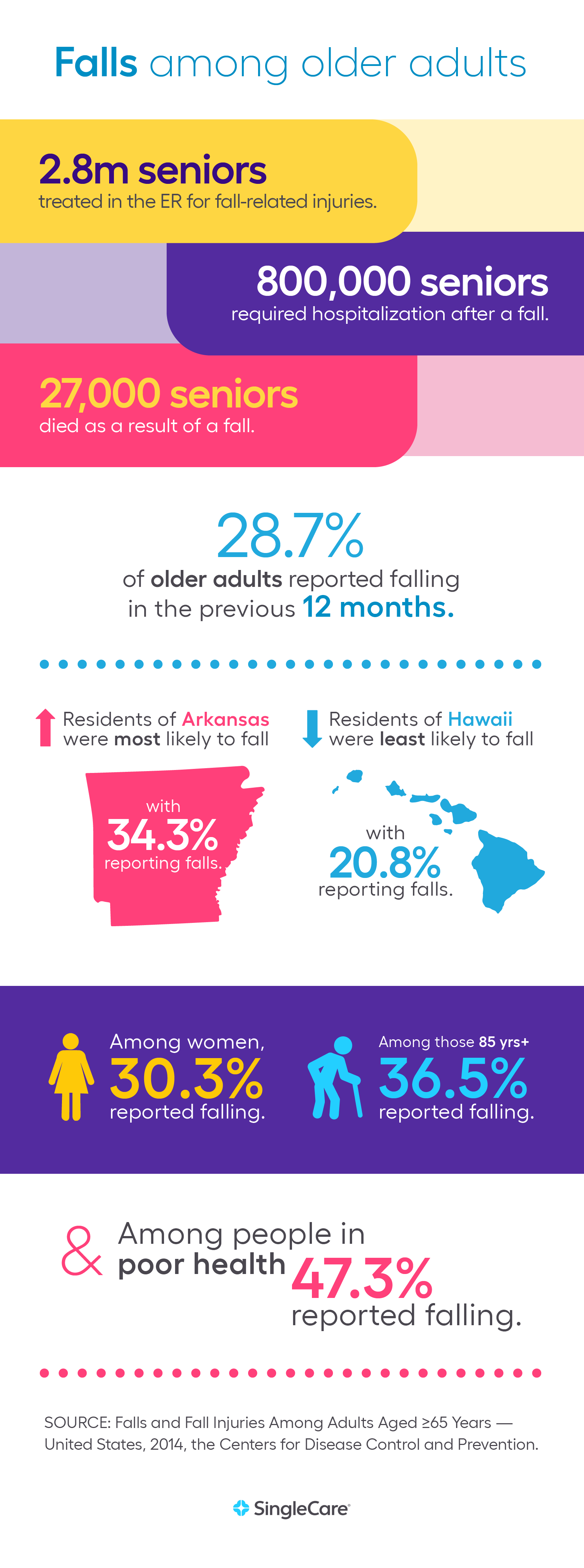
Studies show that 28.7% of older adults fall every year in the U.S. Given today’s population, that’s about 36 million total falls. In an average year, 3 million older Americans go to the emergency room after a fall.
The Centers for Disease Control and Prevention (CDC) reports that falls among seniors are getting more common and more deadly. Death rates from falls have increased 30% in the past 10 years, and by 2030, the CDC expects total falls to increase from 36 million to 52 million.
Thankfully, there are proven measures to help reduce the risk that an older adult will experience a fall.
What is fall prevention?
Fall prevention strategies comprise different areas such as technology, education, physical therapy, and safety devices designed to reduce the risk of falling. Walkers are an example of a fall prevention device. Tai chi is a fall prevention exercise. Medication reviews, which can evaluate whether certain medications or drug interactions are causing excessive drowsiness or dizziness, are a common fall prevention tactic.
What causes seniors to fall?
As we get older, our bodies tend to change in ways that may make us more likely to fall. Even among seniors, the older a senior is, the more likely they are to fall. According to a 2014 survey of seniors by the CDC, 26.7% of those aged 65 to 74 reported having fallen in the past year. Among those aged 75 to 84, 29.8% reported falling, and 36.5% of those 85 and older reported falling.
These are the most common reasons that seniors fall and get injured.
- Diminished eyesight and hearing
- Loss of balance and flexibility
- Weakened muscle and bone strength
- Medication side effects
Diminished eyesight and hearing
Our eyesight gets worse as we age. Eye changes are a part of aging, and they often develop gradually. Normal, aging-related sight changes include seeing in lesser detail, not distinguishing between colors as well, and seeing worse in low-light conditions.
When someone can’t see detail as well, they may miss things like cracks in the sidewalk, or may misjudge the height of a curb.
When someone loses the ability to distinguish between colors, they may not notice changes in surfaces, such as changes from hardwood floor to rug or asphalt to gravel.
Low-light vision problems make early morning, twilight, and evening especially dangerous—even in the home. An item unexpectedly left on the floor, easily visible in daylight, can be the cause of a painful fall.
People who lose their hearing are also more likely to fall, though medical researchers aren’t sure exactly why. One theory is that an inability to hear as well can lead to an overall lack of awareness of the surrounding environment, which can lead to falls. Another possibility put forth by researchers is that because the mind is working so hard to try to hear, it might not have the processing power to help regulate gait and balance.
Loss of balance and flexibility
Mobility issues are not an inevitable consequence of aging. Plenty of older people exhibit outstanding balance deep into old age. Consider this 103-year-old sprinter and 100-year-old marathoner. Nearly all of the time, changes in gait are caused by underlying medical conditions rather than some sort of natural deterioration.
But older people are more likely to have underlying medical conditions that can cause mobility issues. So struggling with balance (or to walk) is, unfortunately, very common among older people. According to a CDC study, 31.7% of people age 65 and older report having difficulty walking three city blocks.
Flexibility may also decrease with age. As a person ages, their muscles might not stretch as much as they used to, making it harder to recover when thrown off balance.
Muscle and bone strength
The natural deterioration of muscle and bone strength as we age often plays a role in the serious injuries that result from falls. As our bodies are starting out, we can fall over and over again with no ramifications—just watch a baby who’s learning to walk. But when we’re older, weaker muscles can lead to falls that can also cause bone fractures.
Hip fractures are among the most serious consequences of falling. A fractured hip completely eliminates mobility, which can lead to further deterioration of the muscles. Sometimes seniors are never able to recover full mobility following a hip fracture. More than 300,000 older Americans suffer hip fractures every year, and 95% of these are caused by falls.
Medication side effects
Medications can make us drowsy or dizzy, and sometimes we don’t even realize that it’s happening. Seniors should ask their doctor or pharmacist whether medications have these side effects. Side effects can be worse for some people, so even if a medication is not supposed to cause a side effect, the medical team should be notified. They may be able to recommend a replacement or a change in dosage to reduce side effects.
According to the CDC, these medications are linked to falls:
Psychoactive medications such as:
- Anticonvulsants
- Antidepressants
- Antipsychotics
- Benzodiazepines
- Opioids
- Sedative-hypnotics
Prescription drugs, over-the-counter medications, and herbal supplements, such as:
- Anticholinergics
- Antihistamines
- Alpha-blockers
- Muscle relaxants
Fall risk assessment for seniors
A fall risk assessment involves a series of questions and physical tasks that are used to determine how likely it is that a senior will fall. The CDC now recommends an annual fall assessment for everyone aged 65 and older.
A medical practitioner will make the assessment. They will ask questions about how the senior perceives their balance to be, and about whether they have fallen or have feared that they were going to fall.
The practitioner will also test and observe the senior with a series of physical tests. One example is called the “Timed Up-and-Go” or TUG test. The practitioner will have the patient sit in a chair approximately 10 feet away from a line or object on the floor. The practitioner will ask the senior to rise from a seated position, walk to the line or object, return to the chair, and sit. A senior who takes longer than 12 seconds to do this is considered at risk of falling.
After the questions and tests, the practitioner will determine whether a senior’s risk of falling is low, medium, or high. If the assessment shows a high risk of falling, medical professionals will offer additional tools, resources, and possibly therapy, to try to reduce the risk.
What can happen when seniors fall?
The worst outcome of a fall is a serious injury leading to a hospital stay. According to the CDC, 800,000 Americans a year are hospitalized because of a fall. Falls can cause hip fractures, traumatic brain injuries, and broken bones that take time to heal.
Recovery time, including physical therapy, can stretch for weeks or months. Sometimes the senior can’t be discharged directly to their home, but must spend additional time in a rehabilitation facility. In some cases, the senior is never able to return home.
But a fall that doesn’t lead to a hospital stay can also be dangerous.
Falls can cause undiagnosed head injuries. A senior may think they are fine, but are actually suffering from a concussion. Undiagnosed head injuries are extremely dangerous for seniors who are taking blood thinners. These drugs, often used to treat or reduce the risk of blood clots, can put seniors at higher risk of internal bleeding in the brain after trauma.
And falling is scary. A senior who has fallen while walking into a restaurant, or using the restroom at a movie theater, or even taking out the trash, may be traumatized by the experience. The fear of falling again may make them want to avoid leaving the house, which could lead to social isolation. It may also make them start to neglect household chores, creating unsafe living conditions.
Prevention is the best medicine. Seniors, their families, and their medical teams can work together to substantially reduce the risk of falling.
Talking with seniors about falling risk
If you are concerned about the risk of a fall for a senior in your life, the first step is to talk with them about their fall risk assessment. Make sure they have taken one in the past 12 months. If they haven’t, make sure that they do one soon. If they don’t remember the results, work with them to find out what the assessment was.
It’s important to start any conversation after the assessment, because not every senior is at high risk for a fall. You wouldn’t tell these mountain climbers in their 60s and 70s to start wearing slip-proof socks around the house since they have better balance than most 20-somethings.
A senior—regardless of age—who has been judged to have a low risk of falling, does not need to start drastically limiting their behavior. Reducing a senior’s physical activity when there’s a low risk of a fall may hurt their quality of life and mental outlook.
It’s a different conversation if the risk assessment does show an elevated risk of falling. This conversation should happen with the person’s medical team, and may include:
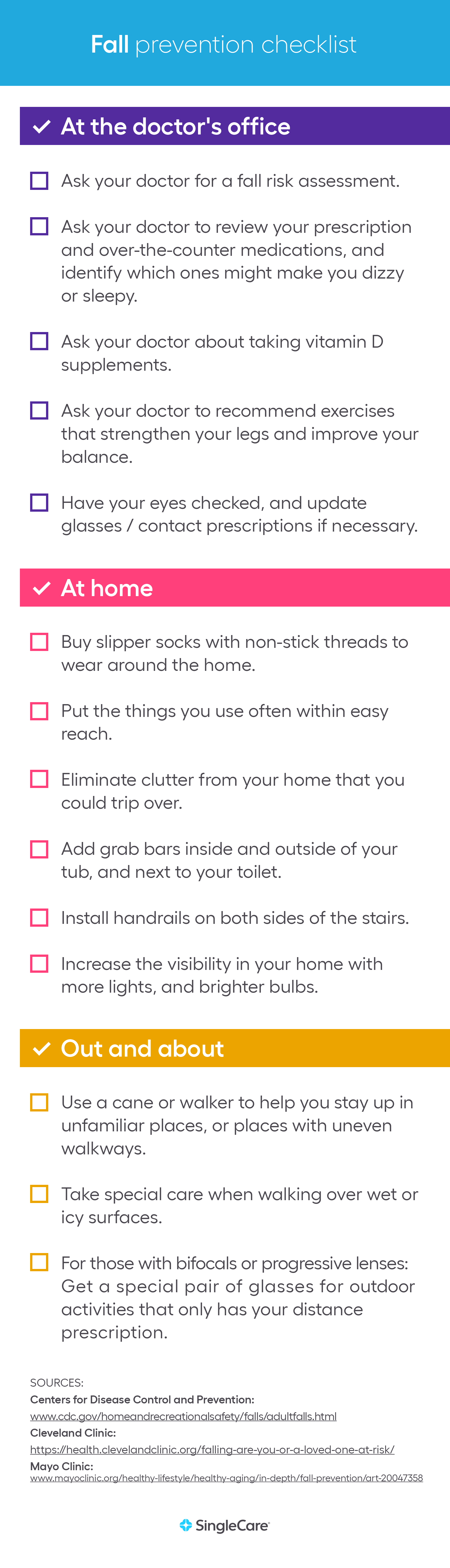
- Assessing the senior’s current prescription and over-the-counter medications to discuss if any cause dizziness, drowsiness, or disorientation.
- Recommending supplements. One common recommendation is vitamin D supplements which can improve muscle strength and function.
- Discussing possible therapy or exercise.
- Scheduling an eye exam.
- Scheduling an in-home visit to identify safety risks.
Fall prevention strategies and best practices for seniors
Seniors and their loved ones can take actions that are proven to reduce the risk of falling.
- Improving the senior’s ability to see
- Improving the senior’s strength and balance
- Making the home a safer place
Eyesight
Seniors need more light wherever they go. In the home, living spaces and walkways should be well-lit with adequate light bulbs and additional lighting as needed. On porches and in yards, outdoor lighting should be added. For example, you could install bright lights along the path the senior uses to take out their garbage.
Seniors at high risk for falling should do solo activities and errands during the day. If a senior with a high risk for falling is out at night, find someone to accompany them.
The senior should also see their eye doctor for adjustments to their prescription and if needed, get new glasses to help reduce the risk of falls. Any senior with progressive lenses or bifocals should get a pair of glasses with their distance prescription only. These glasses can be worn when the senior is doing outdoor activities, and will help them see obstacles like broken sidewalks, curbs, area rugs, and the like.
Strength and balance
A senior’s strength and balance are not predetermined to diminish with age. People of any age can improve their strength and balance through exercise.
There is one community-based exercise program that has been specifically designed for seniors who need to improve their balance: Tai Ji Quan: Moving for Better Balance. The program is based on the practice of tai chi, a Chinese martial art that emphasizes deliberate, flowing movements. The Tai Ji Quan program has modified the traditional movements into a therapy that targets “postural control, daily functioning, and clinical rehabilitation for older adults and individuals with physical limitations.”
Movements, under the guidance of a trained practitioner, are performed in groups, making this an ideal training program for nursing homes, rehab facilities, and senior centers.
For a simple exercise a senior can do at home, the CDC recommends the “Chair Rise Exercise” to strengthen the muscles in the thighs and buttocks.
In this exercise, the senior slowly rises from a chair, using their hands to support them. Once fully standing, they pause, and then slowly return to a sitting position. Then they repeat the exercise 10 to 15 times, if possible.
The goal of the exercise is to have the senior sit and stand while using their hands as little as possible for support.
As the senior works to improve their balance, they can use the support of a cane or walker—especially when traversing uneven surfaces, or unfamiliar terrain.
Home safety
A fall at home can be devastating, especially if there is no one around to help. A senior who is at risk of falls may have to make improvements around the home, or may have to leave their home.
Basic safety improvements for homes may include:
- Grab bar for the shower/bathtub on both the inside and outside
- Grab bar near the toilet
- Handrails for all staircases on both sides
- Removal of throw rugs, mats, or loose area carpets
- Additional lighting
The other home safety improvements are more lifestyle changes. For example, if a senior has a habit of getting up every night to pour themselves a glass of water, they can choose to have a carafe on their nightstand so they don’t have to make a trip to the kitchen. Medications, pantry items, and kitchenware should be removed from high shelves that require step stools for reaching. Store these commonly-used items in more convenient places, such as lower shelves or on a counter.
Home clutter might also contribute to falls. Organize loose items and schedule a cleaning service if necessary.
Preventing seniors from falling helps everyone
Falls among seniors are not only devastating for an individual’s health, they are also very costly for the healthcare system. Approximately $50 billion is spent every year on medical costs related to non-fatal fall injuries in seniors, with $38 billion of that coming from the taxpayer-funded Medicare and Medicaid programs.
Better fall prevention strategies could help lower costs for hospitals, insurers, and the federal government, as well as lower health care premiums and tax bills for everyone. Fall prevention for seniors is important to all of us.




