Key takeaways
Caregiver burnout results from the emotional, physical, and mental exhaustion of caring for someone else’s needs, often leading to caregiver depression if not addressed.
Risk factors for caregiver burnout include physically demanding tasks, financial difficulties, and lacking a support network, among others, with signs including overwhelming stress, sleep issues, and frequent illness.
Strategies to avoid caregiver burnout include taking regular breaks, utilizing online resources and tools for easier communication, joining a support group, and setting personal health goals.
It’s critical for caregivers to practice self-care by setting realistic caregiving goals, seeking professional advice, and developing coping strategies to manage the stress of caregiving effectively.
A caregiver is anyone who assumes a significant level of responsibility for another person. This could be a family member, friend, or home healthcare worker. Caregivers demonstrate selflessness, commitment, and duty every day. But they also take on emotional and physical burdens that can become overwhelming.
What is caregiver burnout?
Caregiver burnout is a state of total exhaustion brought about by the emotional, physical, and mental toll of assuming responsibility for another person’s needs.
How does caregiver burnout start?
In most cases, caregiver burnout begins with emotional exhaustion. The stress and burden of providing for someone’s critical needs can exhaust a person’s ability to cope. Emotions like anger, sadness, and fear can be harder to control than usual.
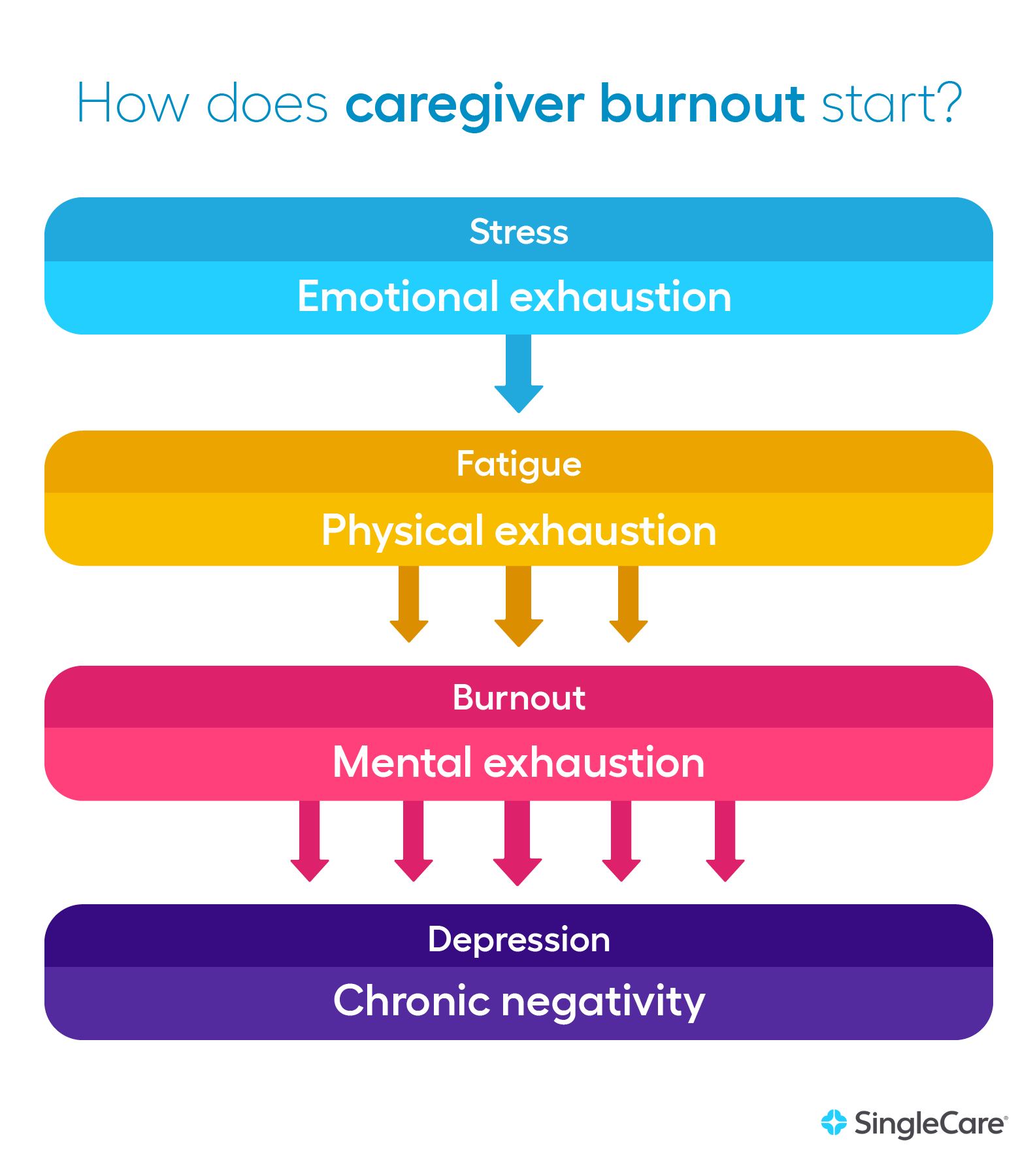
Physical exhaustion often follows. Caregiving often requires new physical demands and usually leads to a reduction in other physical activities like exercise. One person may feel lethargic because they no longer go on their morning walk. Another person may have sore muscles because they have to bathe and clothe someone else, or sleep somewhere unfamiliar.
The combination of emotional and physical exhaustion can lead to mental exhaustion. A caregiver may begin making simple mistakes like forgetting appointments or leaving a key ingredient out of a favorite recipe. Restful sleep may be difficult, and a caregiver may lack motivation for social interaction. This is when exhaustion has reached the burnout stage.
If caregiver burnout is not addressed, it can lead to caregiver depression—a dangerous situation for the caregiver and the person to whom they are giving care. Depression is often characterized by feelings of worthlessness, sadness, or irritation, which can sometimes lead to chronic negative thoughts of hurting themselves or others.
If you or a loved one is experiencing severe depression or suicidal thoughts and behaviors, seek help from a healthcare provider or emergency room immediately. You can also call the National Suicide Prevention Lifeline at 800-273-TALK (8255).
Why is caregiving so exhausting?
Caregiving is exhausting because of the time and energy it requires. When someone you love can’t entirely fend for themselves, you want to help them. But when you are preparing meals, sorting out their financial situation, or helping them use the bathroom, you are using up energy and hours normally devoted to your own well-being.
In the end, the exhaustion often comes from losing the ability to do things that you enjoy and that make you, you.
What are the risk factors of caregiver burnout?
Not all caregivers get caregiver burnout. But among those that do, researchers have identified certain risk factors that seem to make caregivers more likely to suffer from burnout. Not everyone who has these risk factors will experience burnout, and people who don’t have any of these factors may experience burnout anyway.
Still, it is worth reviewing these risk factors and being aware of any that apply to you.
- Physically demanding tasks (i.e., lifting someone out of a bathtub)
- Taking care of someone that has severe behavior problems (i.e., dementia), not only physical ones
- Financial difficulties
- Living with the person you’re caring for
- Lacking friends or a support network
- A high percentage of time or long duration spent as a caretaker
- History of substance abuse
What are the signs of caregiver burnout?
Certain signs may indicate total exhaustion or caregiver burnout. If you are a caregiver or know someone who is a caregiver, look for the following signs.

- Feeling overwhelmed
- Feeling constantly worried
- Not getting enough sleep, or sleeping too much
- Gaining or losing weight
- Feeling angry at the person you’re caring for
- Feeling easily irritated
- Avoiding friends and family
- Feeling sad or hopeless
- Having frequent body pains, such as headaches
- Increasing the use of alcohol, drugs, or prescription medications
- Getting sick more often
Caregivers experiencing any of these symptoms should speak to their doctor.
Measuring caregiver stress and burnout
The Zarit Burden Interview is the most widely used diagnostic tool for identifying caregiver burden.
To determine whether you are experiencing excessive caregiver stress, consider taking this Caregiver Health Self Assessment Questionnaire that was developed by the American Medical Association.
How to avoid caregiver burnout
You now have an understanding of what caregiver burnout is, how to recognize it, and who is most likely to get it. Here are 12 proven methods of avoiding burnout.
1. Make sure you get breaks for yourself
There’s no “pause button” for caretaking. Every caregiver may have felt the urge to simply walk away, but they understand that doing so could be catastrophic for the person who is relying on them. You don’t want to let it get to that point.
That’s why implementing breaks into your daily routine is so important. Short breaks can have a hugely positive impact on your mental outlook.
In some cases, the person you are taking care of can manage on their own for a few hours, so you can get away. Others may at least be able to entertain themselves safely while you are in another room.
If you are helping someone who needs constant supervision, you’ll have to be proactive about scheduling breaks. This could mean drafting a neighbor, friend, or family member to help periodically. Or it could mean hiring a home healthcare worker to stop in a few days per week.
We’ve already learned that a high percentage of time spent as a caregiver is a risk factor for burnout. Do everything you can to ensure you have time to yourself to relax and recharge. It’s the best thing for you and for the person you’re caring for.
2. Use tools that make sharing updates simpler
A primary caregiver isn’t only a healthcare worker, they’re a reporter, too. Close family and friends will expect updates on topics like symptoms, prognosis, how their medication is working, what the person is eating, and more.
Individual calls or emails are nice, but time-consuming. When a caregiver isn’t able to provide updates as often as they’d like, they can feel guilty about it which adds to their burden.
Tools like CaringBridge, PostHope, or MyLifeLine make communication easier. These sites let you post updates simultaneously—with controls to protect your loved one’s privacy.
A single update shared with everyone also reduces the risk of miscommunication. Everyone will have the same information, so they don’t feel left out.
3. Use online resources
Every caregiver should have a device with internet access. Critical advice and important resources can often be just a few clicks away.
One of many examples is Eldercare Locator. This free resource site, produced by the U.S. Department of Health and Human Services, has a clean, readable design and trustworthy links. In just a few clicks, you can connect with insurance, transportation, and home care resources.
Many other online resources for caregivers are worth consulting, such as online support groups and local home health organizations.
4. Join a support group
Participating in a support group is one of the best ways that a caregiver can use their limited free time. Caregiving can be isolating and frustrating. On the most basic level, a support group reminds caregivers that there are others facing the same challenges.
But on a deeper level, a support group can help provide guidance that’s based on experience. And a caregiver can feel the satisfaction and catharsis of helping others by sharing their successes and failures with other like-minded individuals.
Bonding over these shared experiences often leads to friendship. As supportive as family and friends can be, they can only sympathize with what you’re going through. A fellow caregiver can share the burden and support you, like a coworker or teammate.
5. Take a self-assessment test regularly
Caregiver burnout doesn’t happen all at once. Emotional, physical, and mental exhaustion accumulates over time.
You stand a better chance of avoiding burnout if you track benchmarks in your mental health. Taking a self-assessment test regularly (say, once a month) will give you a clearer view of how well you are coping.
Self-assessments ask basic questions about your feelings and your physical health. They shouldn’t take more than 10 to 15 minutes. We recommend the Caregiver Health Self Assessment Questionnaire, which was developed by the American Medical Association.
This small-time investment could save you the consequences of burnout.
RELATED: How to make and use a self-care checklist
6. Maintain positive relationships with other friends and family
When a loved one is going through a health crisis, everyone wants to help. Sometimes the best help is the simplest: Reaching out to a friend or family member.
Caregivers need a sense of normalcy that can often be obtained by going on a walk with a former coworker, having brunch with old friends, or enjoying a night at the bowling alley.
Friends and family may feel that they have to do extra, or they may feel hesitant about trying to contact you. Try to maintain a schedule with friends and family members, either by having a phone call every few months or arranging lunch meetups once a week.
7. Set boundaries
One of the biggest changes when you become a caregiver is making decisions for someone else. And the people who also love that person may not always agree with the decisions you make.
You can’t make everyone happy, and being second guessed adds to your burden. Family and friends who want to provide help may do so in a way that interrupts your routine.
So set clear boundaries about things like who should attend doctor visits, when people should visit, and the types of assistance you actually need.
8. Set health goals for yourself, including mental health
The emotional burden of caregiving can cause you to neglect your physical and mental health.
Positive behaviors like exercise and meditation become important when you are under emotional strain. They are an effective way to calm your racing thoughts.
Give yourself achievable goals for activities like these. Phone apps can help by providing daily reminders and preset programs that last 10 to 30 minutes.
9. Set realistic goals for your caregiving and ask for help when you need it
Too many caregiving situations start in crisis mode and stay there. That’s a sure path to caregiver burnout.
Early on, work with your doctor to identify a realistic level of caretaking. Think about your loved one’s current and future needs and whether you will be able to provide them.
For example, someone with a progressive, debilitating disease may be able to function normally now, but what happens when they need help getting in and out of the bathtub?
What types of care are you comfortable giving? Could you give shots, or monitor IV drips? What about driving to pick up medications or necessities like groceries with them in the car?
Think about what will go into caretaking in your unique situation, and set realistic goals for what you can do.
Overextending yourself can lead to burnout (or a dangerous situation) for the person you’re caring for.
10. Talk to a professional, including a therapist or social worker
Becoming a caregiver is a time of stress and even shock. These are times when talk therapy can be extremely comforting and critical to our ability to cope.
Family and friends can be a sounding board, but they also have a close relationship with the person you’re caring for. That makes it hard to honestly discuss feelings of shame, guilt, or anger—feelings that are common and valid.
Speaking to a third party gives you the freedom to express yourself, put certain feelings out into the open, and work on strategies for coping with them.
RELATED: How does teletherapy work?
11. Be realistic about your loved one’s disease
Another reason to seek advice from a third party is to be able to honestly discuss your loved one’s path to recovery—or their lack of one.
For dementia patients, sadly, there is no cure. And doctors can’t say for sure how fast the disease will take hold.
Acceptance can be the hardest part of dealing with certain diseases. We want to believe our loved ones will beat the odds. Thinking realistically about what the future holds can help us balance our hopes with the practical requirements of home care.
12. Develop coping strategies that work for you
Every caregiving situation is different and so is every caregiver.
Some people may decide to take time for solitary walks before deciding that what they really want is to join a support group.
Coping on a daily basis can be a real challenge. Try to identify the stressful parts of your day and how you could alleviate that stress. Maybe you’d benefit from getting housekeeping help or a meal delivery service. It doesn’t have to be forever, but keeping your head above water for the health of you and the person you’re caring for has to be the top priority.
Self-care is part of caregiving
Caregiving can be a shock to the system. Our instinct is to help our loved one, no matter the cost to ourselves. But as the days, weeks, and months go by, we run out of energy.
The most important thing for caregivers to remember is this: Successful caregiving includes caring for yourself.




