CORONAVIRUS UPDATE: As experts learn more about the novel coronavirus, news and information changes. For the latest on the COVID-19 pandemic, please visit the Centers for Disease Control and Prevention.
You’ve probably read that 80% of people who get COVID-19 will have mild coronavirus symptoms. But what exactly does that mean? Is a mild case similar to a respiratory illness like the common cold or the seasonal flu? What separates a mild case of coronavirus from a moderate one? What COVID symptoms make a case severe?
Coronaviruses are a family of viruses, but this is a new coronavirus, officially called SARS-CoV-2. This novel coronavirus, also called COVID-19, first surfaced in Wuhan, China, at the end of 2019 and was transmitted to humans from an animal source. Experts have learned, and are still learning, about the different ways it affects people.
One thing experts know for sure: It’s a fairly contagious virus that is spread through aerosols (e.g., airborne particles much smaller than droplets that linger in air) as well as droplets (e.g., the sneezes and coughs) of infected people. Touching respiratory droplets as well as touching an infected person, will also transmit the virus. This is why handwashing, social distancing, self-isolation, and vaccination are so important in slowing coronavirus transmission.
RELATED: Does hand sanitizer expire?
Prevalence of mild, moderate, and severe COVID-19 cases
The latest research indicates that the vast majority of COVID-19 cases fall into the least severe category:
- Mild to moderate: 81%
- Severe: 14%
- Critical: 5%
Age seems to be a strong factor in who gets the sickest. In a recent analysis of coronavirus disease 2019 in the United States, the Centers for Disease Control and Prevention (CDC) found that older people have the highest death rate.
It’s important to note, however, that while older people are most likely to die from the disease, young people are not immune to COVID-19.
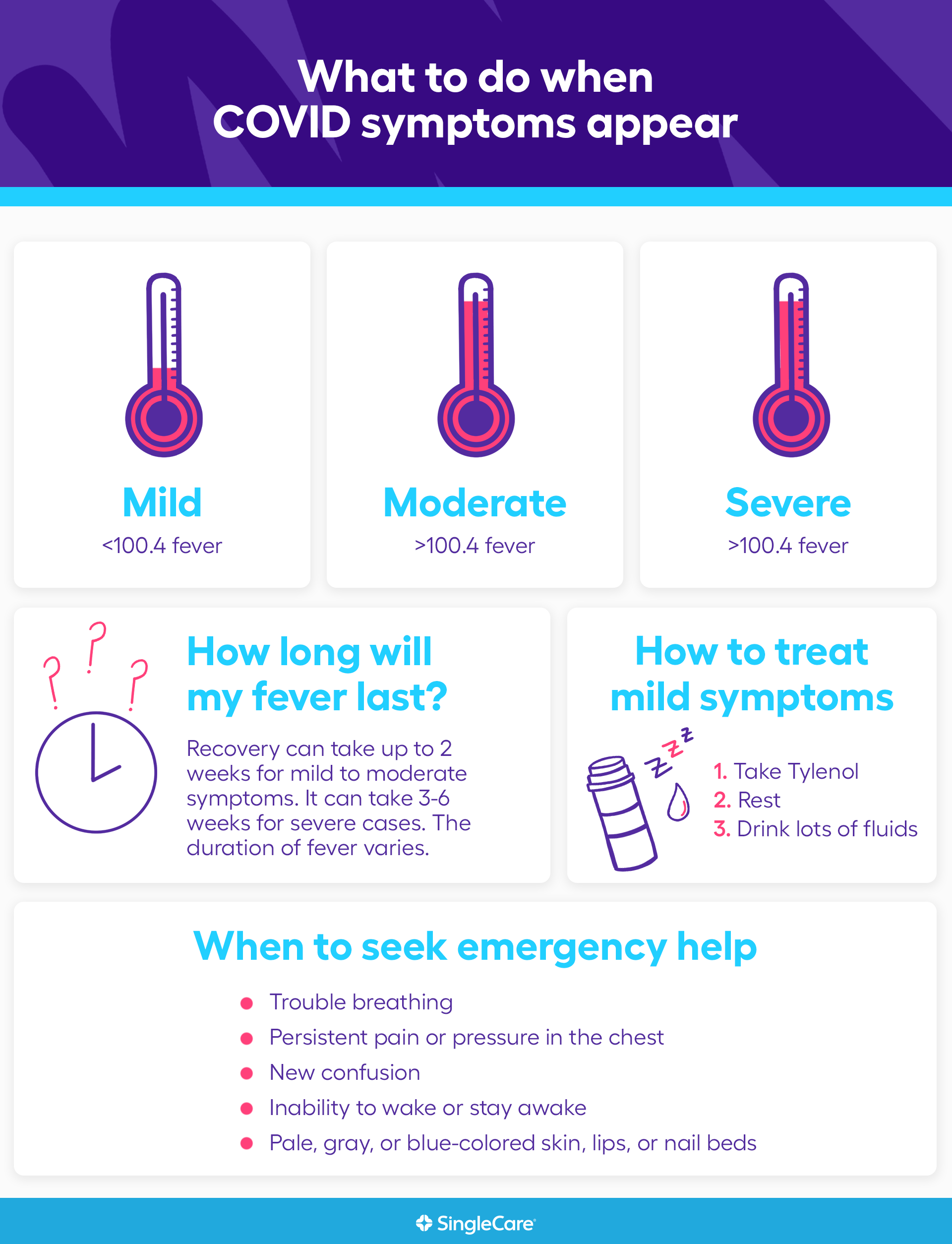
Coronavirus symptoms: Mild vs. moderate vs. severe
How your body responds to this new coronavirus infection depends on your:
- Age
- Immune system
- General health
- Any underlying health conditions
Conditions such as diabetes, lung, kidney or heart disease, high blood pressure, and obesity can make you more vulnerable to COVID-19.
It’s possible to have the infection and not show any coronavirus symptoms at all.
According to the CDC, 30% of COVID cases can be asymptomatic.
Mild symptoms
Most people infected with the virus will have mild respiratory illness symptoms such as nasal congestion, runny nose, and a sore throat. Other mild symptoms of COVID-19 include:
- Low-grade fever (around 100 degrees Fahrenheit)
- Dry cough
- Fatigue
- Headache
- New loss of taste or smell
- Gastrointestinal upset, including vomiting and diarrhea
- Itchy, painful patches on skin (especially in young people). These patches often show up on the toes and have been referred to as “COVID toes.”
“With a mild case, you might feel as though you have a cold,” says Carl J. Fichtenbaum, MD, professor of clinical medicine at the University of Cincinnati College of Medicine. “The symptoms are annoying, but you feel as though you can carry on with most of what you need to do without feeling too impaired.”
Moderate symptoms
- Fever of >100.4 degrees Fahrenheit
- Chills, with repeated shaking
- Deep cough
- Fatigue and body aches
- Muscle pain
- General feeling of being unwell
- Some shortness of breath
“These people will have some of the same symptoms as those with a mild case of COVID-19, but the fever may be a little higher, the coughing deeper, and they may feel more rundown,” notes Dr. Fichetenbaum. “They’ll generally feel sicker.”
Severe symptoms
Some or all the common COVID symptoms mentioned above along with:
- Shortness of breath, even when you’re not exerting yourself
- Chest discomfort
- Confusion/unresponsiveness
- Trouble staying awake
- Eye problems, such as watery eyes or swollen eyelids
- Bluish face/lips (a sign you’re not getting enough oxygen)
Breathing issues are a medical emergency. Call your healthcare provider or 911 for immediate guidance. COVID-19 can lead to pneumonia and lung scarring.
RELATED: Is pneumonia contagious?
Coronavirus incubation period and recovery time
The COVID incubation period—the time between when you’re infected with the virus and when symptoms start—is two to 14 days, with a median of four to five days. Research shows that the vast majority of people infected with the virus will start to show symptoms by about 11 to 12 days. Recovery for those with severe cases can take three to six weeks, and even longer in some cases.
It’s possible to start out with a mild case of coronavirus and have it turn severe. “The timing of this will depend on each individual’s immune system and underlying health conditions. There have been reports of symptoms developing very rapidly, over the course of hours, and other cases that take days to evolve,” says Libby Richards, Ph.D., RN, CHES, associate professor at the Purdue University School of Nursing.
Can you get reinfected with the virus after you recover? Experts are still researching this. But the CDC does say that reinfection with COVID-19 is highly unlikely in the first three months after you’ve been infected.
Coronavirus treatments
While scientists have developed COVID vaccines, as of now, there’s no “cure” for the infectious disease. Treatment for mild to moderate cases of this coronavirus involves what doctors call supportive care.
That includes rest, drinking lots of fluids, and taking over-the-counter pain and fever relievers, like Tylenol. More severe cases, especially when there’s difficulty breathing, may need hospitalization. “We’ll want to evaluate these people,” says Dr. Fichtenbaum. “We’ll want to see what their oxygen levels are, if they’re well hydrated, and if they’ll need help breathing with respirators or mechanical ventilators.”
RELATED: Current COVID-19 treatments
When to go to the doctor
The CDC advises people to call their healthcare providers if they think they may have been exposed to the coronavirus and also develop a low-grade fever, cough, or slight shortness of breath. It’s important to call first so the staff can take measures to safeguard their own health and that of other patients if they want you to come in.
Not all fevers or coughs will be due to the coronavirus. To help you get a better grasp of whether you might be suffering from COVID-19 or another respiratory illness, the University of Maryland Medical System advises you ask yourself the following:
- Do you have COVID-19 symptoms?
- Have you visited an area that has high community transmission of COVID 19?
- Have you had close contact with a person known to be infected with COVID-19 (e.g., have you spent extended periods of time i.e., 10 minutes or more with a person with a confirmed case of coronavirus and have you had less than six feet separating you)?
- Are you at higher risk for contracting the coronavirus? For example, are you an older adult, especially one with a severe illness or chronic disease?
If you’re having any of the symptoms suggesting a severe case of COVID-19, contact your healthcare provider immediately, or dial 911. Tell the person you speak with that you think you may have COVID-19. Put on a face mask before help arrives or you leave to seek help. Keep at least six feet away from your family members to avoid the spread of infection.
Compare coronavirus symptoms |
|||
|---|---|---|---|
| Mild cases of COVID-19 | Moderate cases of COVID-19 | Severe cases of COVID-19 | |
| Possible symptoms | Low-grade fever, dry cough, fatigue, digestive issues, loss of taste and smell, itchy, painful skin patches (aka COVID toes) | Fever, deeper cough, fatigue, body aches | Fever, deep cough, fatigue, body aches, breathing difficulties, chest discomfort, confusion/unresponsiveness, bluish lips |
| General fever range* | <100.4 fever | >100.4 fever | >100.4 fever |
| Prevalence | 81% of COVID-19 cases | 14% of COVID-19 cases | 5% of COVID-19 cases |
| Incubation period | 2-14 days | 2-14 days | 2-14 days |
| Treatment | Rest, fluids, over-the-counter pain and fever reducer | Rest, fluids, over-the-counter pain and fever reducer | May need hospitalization for IV fluids, oxygen, antiviral medication, dexamethasone, and help with breathing |
| Recovery | 2 weeks | 2 weeks | 3-6 weeks or more |
* Not everyone experiences a fever with COVID. The normal body temperature range is 97 to 99 degrees Fahrenheit. Fevers may also come and go during a COVID-19 infection. Symptoms may overlap and you may not fall strictly into one category. It’s important that you get medical help and take a COVID test. You should remain isolated for 10 days since symptoms first appeared and until you are fever-free for 24 hours without the use of fever-reducing medications and other coronavirus symptoms are improving.




